Why Biopreservation of Apheresis-Derived Cells Matters in Modern Immunotherapy
The field of cell-based immunotherapy necessitates stringent quality control and preservation methodologies to ensure the integrity, viability, and functional consistency of apheresis-derived cellular substrates. Apheresis, the selective extraction of specific hematopoietic and immune cell populations, underpins the foundational processes of numerous adoptive cell therapies. However, intrinsic variability in apheresis-acquired cellular materials introduces significant challenges, affecting downstream manufacturing reproducibility and clinical efficacy.
With the continuous expansion of approvals and outreach of commercialized advanced cell-based therapeutics, the urgency for harmonized and standardized practices also continues to grow. Variability in how cells are collected, processed, and preserved can significantly impact the consistency and quality of the final therapeutic product. Establishing more uniform protocols – particularly around apheresis collection, handling, processing, and storage is critical to improving the scalability and reproducibility of cell therapy manufacturing.
Managing Variability in Apheresis-Derived Cells
One of the most pressing concerns in this domain is the post-collection heterogeneity of cellular inputs, wherein patient-specific and procedural variables contribute to inconsistencies in the final therapeutic product. Factors such as donor physiology, apheresis protocols, processing kinetics, and preservation conditions all modulate cell yield, viability, and functional properties. These inconsistencies create obstacles not only for manufacturing efficiency, but also for ensuring consistent therapeutic outcomes.
To reduce this variability, it’s critical to establish and implement standardized parameters at every stage – from collection to processing to storage. Organizations like the Standard Coordinating Body (SCB) and Parenteral Drug Association (PDA) are leading efforts in defining best practices in areas like cryopreservation, aiming to bring greater clarity and consistency across the field.1
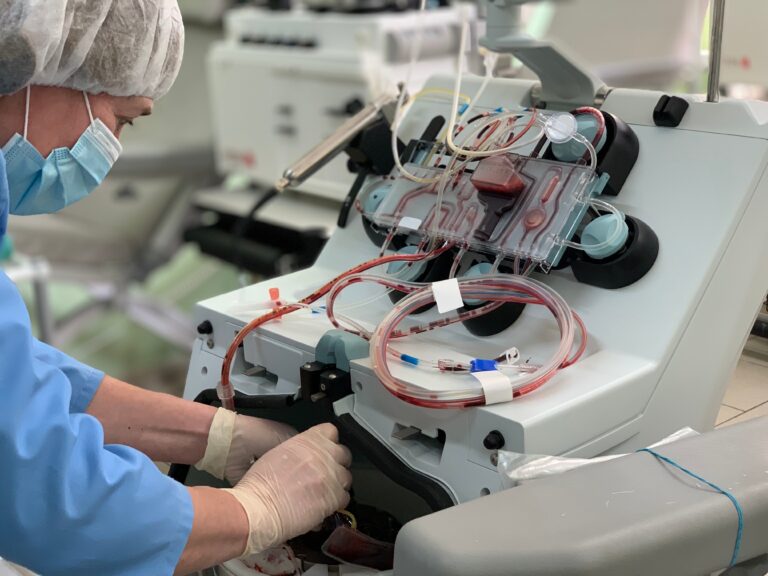
Innovating Biopreservation to Improve Consistency
To address the challenges introduced by input variability, the scientific community has explored and implemented advanced biopreservation strategies aimed at stabilizing apheresis-derived cellular products throughout the manufacturing and distribution process. These strategies are designed to preserve cellular integrity and function across the full vein-to-vein workflow – from initial collection to final infusion.
BioLife Solutions, in collaboration with partners across the regenerative medicine and immunotherapy sectors, has prioritized the optimization of cryopreservation and non-frozen hypothermic storage conditions. These efforts are intended to reduce cellular degradation and sustain viability over time, helping ensure that therapies remain potent, consistent, and ready for clinical use when needed.
Advanced Preservation Media for Enhanced Cell Stability
Recent innovations in cryopreservation and hypothermic preservation have demonstrated strong potential in improving the stability of apheresis-derived cell products. Proprietary biopreservation media such as CryoStor® CS10 and HypoThermosol® FRS have been systematically evaluated for their ability to mitigate cold-induced damage, sustain metabolic activity, and preserve immunophenotypic integrity during transit and prolonged storage.
For example, a study by Shu et al. demonstrated the successful use of CryoStor CS10 in preserving apheresis-derived NK cells for adoptive immunotherapy, highlighting how optimized cryopreservation protocols can maintain viability and functionality of immune effector cells during manufacturing and storage.
Research by Wang et al. demonstrated that cryopreserved leukopaks maintained over 99% cell viability and preserved the functionality of lymphocytes, including T-cells, B-cells, and natural killer cells, suggesting that cryopreserved leukopaks can serve as a viable alternative to fresh collections in cell therapy logistics.
Incorporating specialized preservation solutions into apheresis workflows is a crucial step toward establishing uniformity in cellular starting material across diverse immunotherapeutic applications.
Tailoring Biopreservation Methods for Immune Cell Applications
Conventional cryopreservation methods typically utilize dimethyl sulfoxide (DMSO) as a cryoprotectant, leveraging freezing protocols initially developed for hematopoietic stem cells. However, applying these same approaches to apheresis-derived immune cells often falls short. Different cell types have unique sensitivities and stress responses, and a one-size-fits-all method may compromise cell viability and post-thaw functionality.
To address this, the field is shifting toward cell-type-specific preservation strategies that reduce apoptosis, minimize osmotic stress, and preserve post-thaw functionality. Similarly, non-frozen storage modalities must ensure that collected cells remain metabolically active and functionally competent under rigorously controlled hypothermic conditions.
These customized approaches are reinforced by studies like Gniadek et al., which showed that storing peripheral blood-derived mononuclear cells at 2–8°C in HypoThermosol® FRS preserved viability more effectively than room temperature storage. Findings like these underscore the value of rigorously controlled hypothermic conditions tailored to specific cell populations.
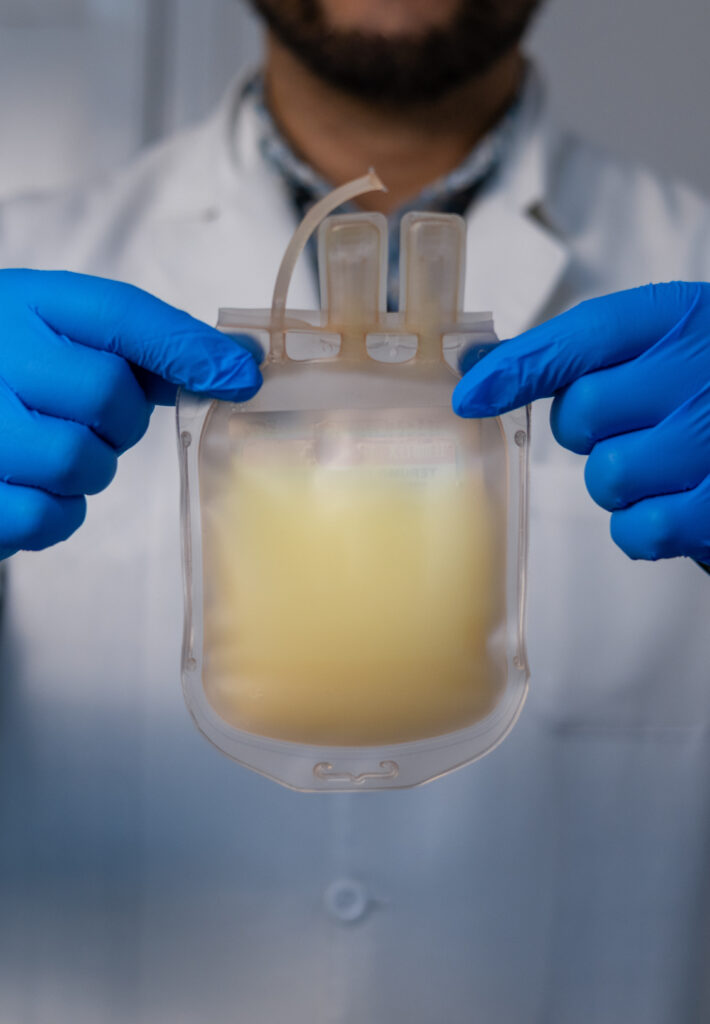
Looking Ahead: Advancing Preservation to Support Scalable Cell Therapies
As cell-based manufacturing continues to scale, the refinement of biopreservation technologies for apheresis-derived starting materials will play a pivotal role in ensuring the clinical and commercial success of next-generation cell therapies.
Collaboration across the ecosystem – including apheresis collection centers, biopreservation technologists, and immunotherapy developers – will be integral to advancing standardized preservation framework that enhances product consistency, maintains therapeutic potency, and expands patient accessibility.
Through ongoing research, technological advancements, and concerted industry efforts, the field is well-positioned to overcome current preservation challenges and support the global demand for scalable, reproducible, and clinically effective immunotherapy treatments.
Conclusion
In the fast-evolving landscape of immunotherapy, optimizing how we preserve and handle apheresis-derived cells is no longer optional – it’s foundational. Standardized, well-validated biopreservation strategies not only improve product consistency, but also support the long-term success of cell therapies in real world clinical settings.
As industry leaders continue to collaborate and innovate, the potential to streamline workflows, reduce variability, and deliver life-changing therapies to more patients becomes increasingly achievable.
Interested in learning more about how BioLife Solutions may help optimize your biopreservation methodologies? Reach out to our team of scientists or explore our biopreservation solutions designed to support the next generation of cell-based therapies.
References
- Parenteral Drug Association. (2021). Cryopreservation of Cells Used in Cell Therapy and Regenerative Medicine Manufacturing (ANSI/PDA Standard 02-2021). PDA. https://www.pda.org/bookstore/product-detail/6498-ansi-pda-standard-02-2021
- Shu, Z., Heimfeld, S., Gao, D., Shi, Y., Pang, W. W., & Hwang, W. Y. K. (2014). A systematic examination of hematopoietic and natural killer cell recovery post-cryopreservation using integrative analytic techniques. Cytotherapy, 16(11), 1400–1411. https://doi.org/10.1016/j.jcyt.2014.04.003
- Wang, W., Hexom, T., Nucho, L.-M., & Eastwood, G. (2015). Cryopreserved leukopaks maintain cell viability and functionality: A solution for cell therapy logistics. Poster presented at the International Society for Cellular Therapy (ISCT) Annual Meeting.
- Gniadek, T. J., Garritsen, H. S. P., Stroncek, D., Szczepiorkowski, Z. M., McKenna, D. H., & Biomedical Excellence for Safer Transfusion (BEST) Collaborative. (2018). Optimal Storage Conditions for Apheresis Research (OSCAR): a Biomedical Excellence for Safer Transfusion (BEST) Collaborative study. Transfusion, 58(2), 461–469. https://doi.org/10.1111/trf.14429
Additional Resources
- Lou Juliano, George Eastwood, Todd Berard, Aby J. Mathew. The Importance of Collection, Processing and Biopreservation Best Practices in Determining CAR-T Starting Material Quality. Cell Gene Therapy Insights 2018; 4(4), 327-336. doi: 10.18609/cgti.2018.032
- Pagliarulo, N. In CAR-T, manufacturing a hurdle Novartis has yet to clear. BioPharma Dive. Dec 6, 2018: https://www.biopharmadive.com/news/ in-car-t-manufacturing-a-hurdle-novartis-has-yet-to-clear/543624/
- Kao, et al. Validation of short-term handling and storage conditions for marrow and peripheral blood stem cell products. Transfusion. 2011 Jan;51(1):137-47. doi: 10.1111/j.1537-2995.2010.02758.x.
- Nicoud, Clarke, Mathew, Rice. Materials and methods for hypothermic collection of whole blood. USPTO 8,642,255; PCT/US2009/038634.